Stoma Basics
Resource and Education Materials
The Stoma
Following surgery, and for as long as the patient has a colostomy, ileostomy, or urostomy, effluent (stool or urine) will exit the body through the stoma and a system for collection and protection of the surrounding skin is required. These are ostomy appliance systems. No two stomas are exactly alike. Each stoma, depending upon it's size and shape, presents its own unique challenges for the caregiver and patient. This section will give you an overview of how to identify which type of stoma your patient has and how to best care for it.
All liquid or semi-liquid effluent can damage skin when soilage remains in contact with skin over time. Urine and ileostomy drainage in particular since it has a high content of digestive enzymes are particulary caustic and can irritate and denude peristomal skin more quickly than solid waste. The use of a skin barrier that fits the stoma snugly and a good collection pouch is essential to maintaining healthy peristomal skin.
Stomas have no nerve endings and do not transmit pain. They are, however, rich with blood vessles and may bleed slightly if rubbed or irritated.
Different Stoma Types:
- Protruding Stoma
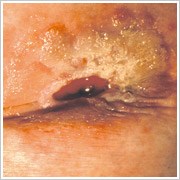
- Flush Stoma
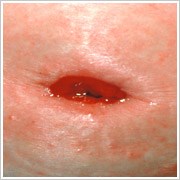
- Retracted Stoma
Need more information? Call Today +65 6245 9838 / +65 9125 1523 or Email to EnquiriesSG@convatec.com
Accessory Tips
The use of ostomy accessories can make meeting the special needs of each one of your patients living with an ostomy easier. Here are some helpful tips about the accessory products from ConvaTec.
- Stomahesive® Paste
- Stomahesive® Protective Powder
Managing Peristomal Skin Issues
At some point, you may encounter a patient who has unhealthy peristomal skin. Identifying the skin issue is the first step in management. Here are some common peristomal skin issues and some general information about them. Click on the links below to view information on Symptoms and Suggested Management Options.
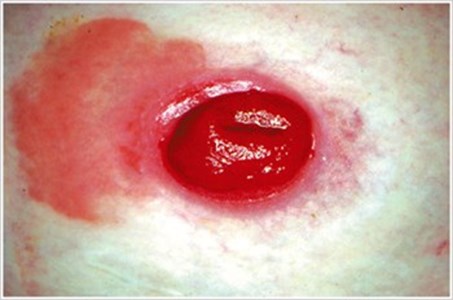
CandidiasisDescription/Causes: Often caused by leakage, perspiration, antibiotic therapy, warm climates, broken skin.
|
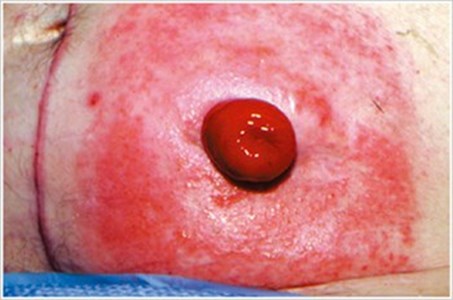
Allergic Contact DermatitisDescription/Causes: Often caused by exposure to materials and compounds that irritate or sensitize the skin on contact (e.g., tape, skin barriers, soap, adhesives, powders, pastes, or pouch material).
|
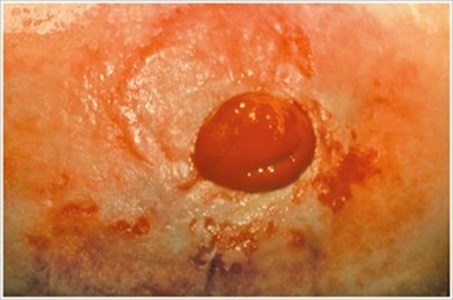
Irritant Dermatitis
Description/Causes:
Inflammation of peristomal skin resulting from contact with stool or urine, usually from leakage under the pouching system.
Symptoms:
- Redness
- Pain
- Weeping areas of skin
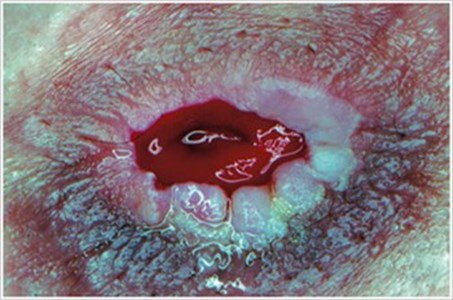
Pseudoverrucous Lesions
(Hyperplasia commonly called PEH)
Description/Causes:
Often caused by chronic exposure of the skin to urine due to an excessively large opening in the skin barrier.
Symptoms:
- Pain
- Wart-like, gray or purple-colored thickened areas next to the stoma
- Frequent leakage or bleeding
- White, sandy, or gritty granules on stoma or around base

Folliculitis
Description/Causes:
An inflammation within a hair follicle caused by traumatic hair removal (e.g., "ripping" skin barrier from skin, shaving too closely, or excessive rubbing or cleaning of peristomal skin).
Symptoms:
- Reddened, pinpoint, or infected areas at the base of the hair follicles around the stoma.
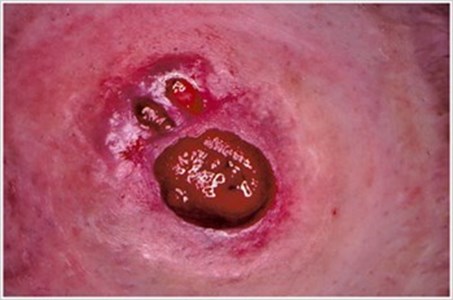
Pressure UlcerDescription/Causes: An ulcer in the peristomal area caused by excessive pressure from an ostomy appliance belt, tight clothing, rigid faceplate, peristomal hernia, or work-related habits. Symptoms:
|
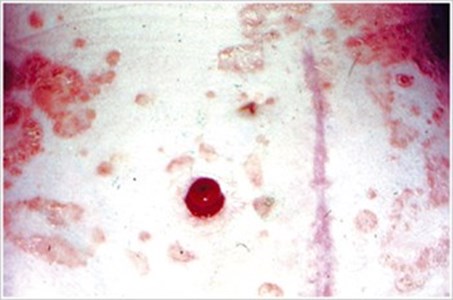
PsoriasisDescription/Causes: A common skin disorder that can occur underneath ostomy pouching systems. Symptoms:
|
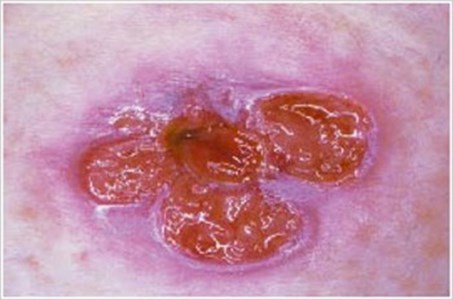
Pyoderma GangrenosumDescription/Causes: An inflammatory skin disease often seen in patients with inflammatory bowel disease ( IBD ) such as Crohn's disease or ulcerative colitis. Symptoms:
|
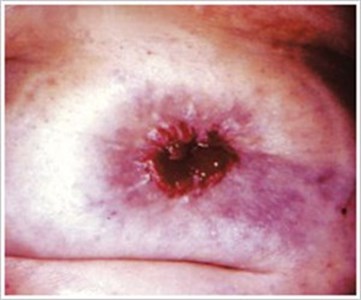
Caput Medusae
Description/Causes:
Refers to a bluish-purple discoloration of the skin caused by dilation of the cutaneous veins around the stoma (peristomal varices).
Symptoms:
- Blue/purple area surrounding the stoma that when blanched, displays irregular, small blood vessels.